Rheumatic fever — first episode hospitalisations
First episode rheumatic fever hospitalisation data and statistics from financial years 2007/2008 to 2024/2025.
On this page
- How we are doing
- Graphs showing annual rates of first episode hospitalisation
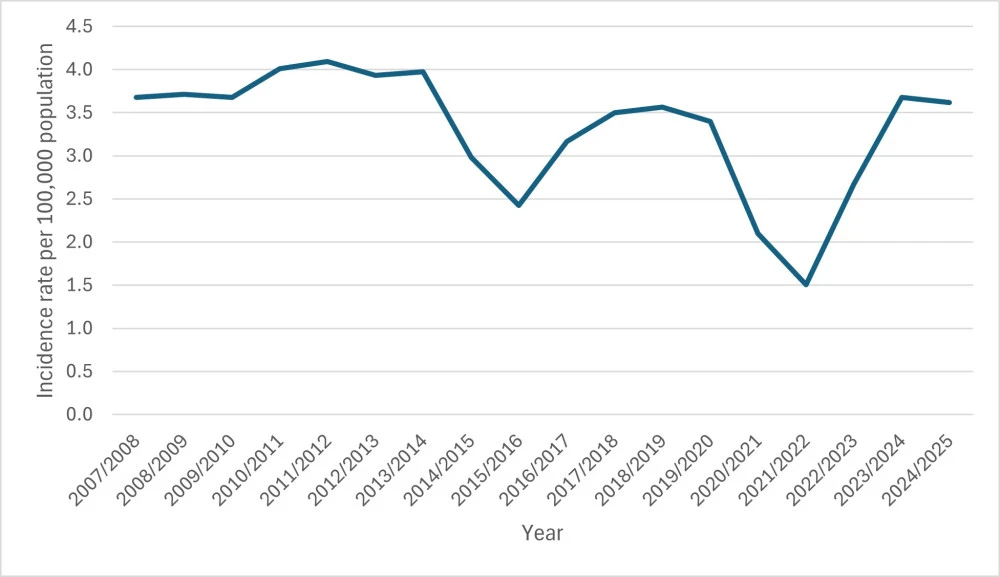
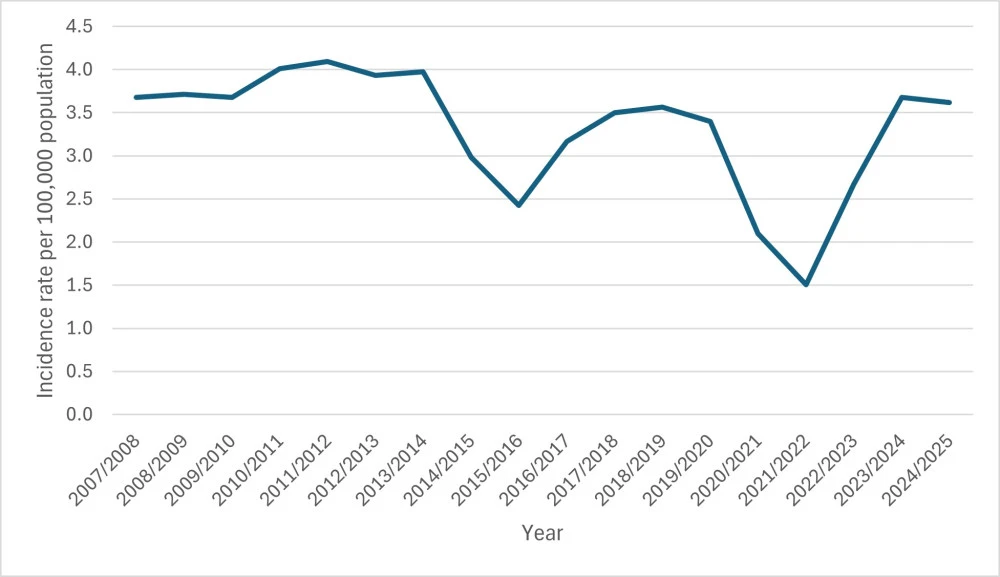
- Annual rate of first episode rheumatic fever hospitalisations per 100,000 people
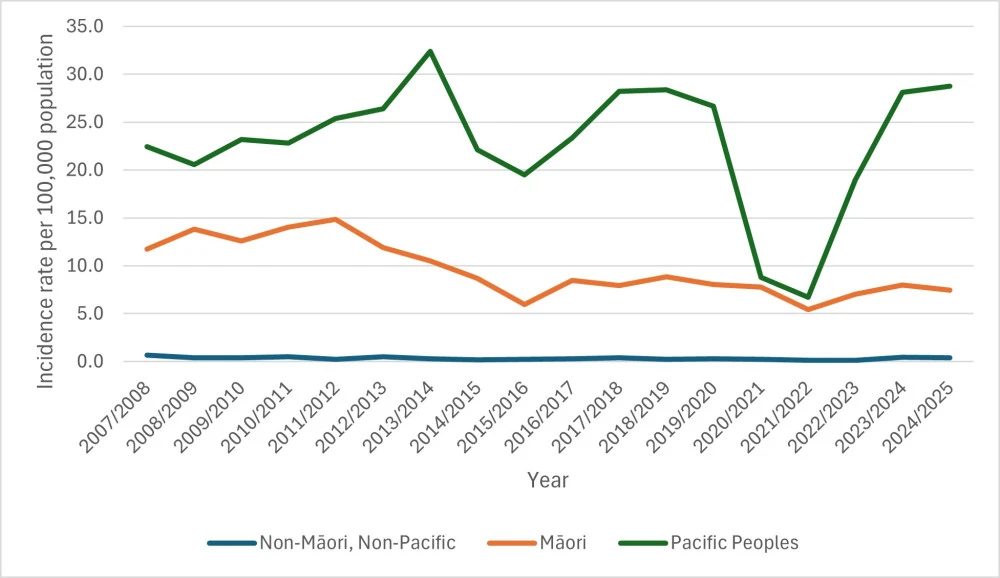
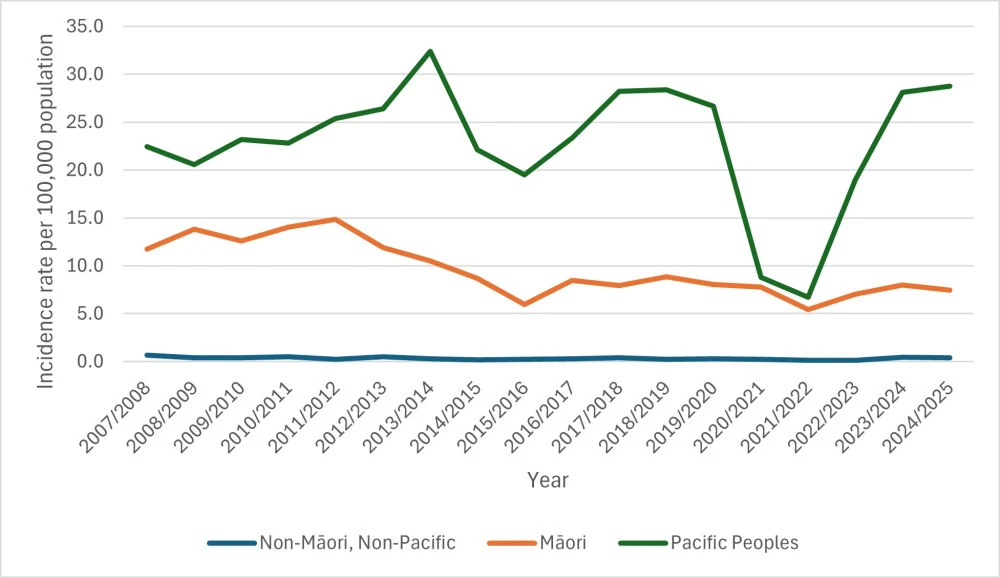
- Annual rate of first episode rheumatic fever hospitalisations per 100,000 people by ethnic group
- First episode rheumatic fever hospitalisations annual total rates and rates by ethnicity — 2007/2008 to 2024/2025
- First episode rheumatic fever annual hospitalisations by age group, district and region — 2024/2025
- Rheumatic fever report
- Rheumatic fever 2024 insights report
- Rheumatic Fever Roadmap 2023 to 2028
Data on this page is sourced from the National Minimum Dataset. 2024/2025 data presented includes 1 July 2024 to 30 June 2025.
How we are doing
In 2024/2025, 194 people were admitted to hospital for the first time with rheumatic fever — 3.62 per 100,000 people. This number has stayed the same since 2023/2024, with the rate of hospitalisation similar to that experienced in 2018/2019 and returning to pre-COVID-19 levels.
Following a decrease in the rate of first-time hospitalisations with rheumatic fever for Māori between 2011/2012 and 2015/2016, this rate has fluctuated between 5.4 and 8.9 per 100,000 people over the last 10 years.
First-time rheumatic fever hospitalisations for Pacific peoples have fluctuated quite strongly since 2007/2008. In 2021/2022 the hospitalisation rate for Pacific peoples was the lowest since 2007/2008. Over the last 3 years the rates have increased. The rate in 2024/2025 being comparable to the previous peak in 2018/2019.
The annual number of non-Māori and non-Pacific people admitted to hospital with rheumatic fever for the first time is low. The rate of hospitalisation over the relevant period was lowest in 2021/2022 at 0.12 per 100,000 people. However, rates for more recent years have been higher at 0.4 per 100.000 people in 2024/2025. In 2024/2025:
- Māori were 18 times more likely to be hospitalised for the first time with rheumatic fever than non-Māori, non-Pacific peoples
- Pacific peoples were almost 70 times more likely to be hospitalised for the first time with rheumatic fever than non-Māori, non-Pacific peoples.
It is also important to note that while New Zealand has higher rates of rheumatic fever compared to other developed countries, the annual numbers are small. Therefore, changes year-to-year may be real, or they may be an artifact of the variability seen when there are small numbers of cases.
In response to the COVID-19 pandemic, a range of public health restrictions were put in place. This led to a decrease in a range of infectious diseases during this period, including a reduction in Group A streptococcus (GAS) related diseases such as rheumatic fever. Once these public health restrictions were removed, the rates of rheumatic fever cases returned to pre-pandemic levels. We will continue to watch the situation closely.
Graphs showing annual rates of first episode hospitalisation
First episode rheumatic fever hospitalisations annual total rates and rates by ethnicity — 2007/2008 to 2024/2025
The table shows the rate per 100,000 people admitted to hospital with rheumatic fever for the first time from financial years 2007/2008 to 2024/2025.
| Financial year | Rate per 100,000 |
| 2007/2008 | 3.7 |
| 2008/2009 | 3.7 |
| 2009/2010 | 3.7 |
| 2010/2011 | 4 |
| 2011/2012 | 4.1 |
| 2012/2013 | 3.9 |
| 2013/2014 | 4 |
| 2014/2015 | 3 |
| 2015/2016 | 2.4 |
| 2016/2017 | 3.2 |
| 2017/2018 | 3.5 |
| 2018/2019 | 3.6 |
| 2019/2020 | 3.4 |
| 2020/2021 | 2.1 |
| 2021/2022 | 1.5 |
| 2022/2023 | 2.7 |
| 2023/2024 | 3.7 |
| 2024/2025 | 3.6 |
The table shows the rate per 100,000 people admitted to hospital with rheumatic fever for the first time from financial years 2007/2008 to 2024/2025 by ethnicity.
| Financial year | Māori | Pacific peoples | Non-Māori, non-Pacific peoples |
| 2007/2008 | 11.7 | 22.4 | 0.7 |
| 2008/2009 | 13.8 | 20.6 | 0.4 |
| 2009/2010 | 12.6 | 23.2 | 0.4 |
| 2010/2011 | 14 | 22.8 | 0.5 |
| 2011/2012 | 14.9 | 25.4 | 0.2 |
| 2012/2013 | 11.9 | 26.4 | 0.5 |
| 2013/2014 | 10.5 | 32.4 | 0.3 |
| 2014/2015 | 8.7 | 22.1 | 0.2 |
| 2015/2016 | 6 | 19.5 | 0.2 |
| 2016/2017 | 8.5 | 23.4 | 0.3 |
| 2017/2018 | 8 | 28.2 | 0.4 |
| 2018/2019 | 8.9 | 28.4 | 0.2 |
| 2019/2020 | 8.1 | 26.7 | 0.3 |
| 2020/2021 | 7.8 | 8.8 | 0.2 |
| 2021/2022 | 5.4 | 6.7 | 0.1 |
| 2022/2023 | 7 | 19 | 0.2 |
| 2023/2024 | 8 | 28.1 | 0.4 |
| 2024/2025 | 7.4 | 28.7 | 0.4 |
First episode rheumatic fever annual hospitalisations by age group, district and region — 2024/2025
The following table shows the numbers and rates of people being admitted to hospital with rheumatic fever for the first time in 2024/2025 by age group. It shows that the majority of cases continue to occur in tamariki between 5 and 14 years — 54%.
| Age group | Numbers | Rate per 100,000 |
| 0 to 4 years | Less than 10 | – * |
| 5 to 14 years | 105 | 15.7 |
| 15 to 24 years | 41 | 6.1 |
| 25 to 44 years | 38 | 2.5 |
| 44 years and older | Less than 10 | – * |
* Rates are not presented for age groups where there were fewer than 10 cases. This is to make sure privacy and confidentiality is maintained.
The following table details the number and rates of people being admitted to hospital with rheumatic fever for the first time in 2024/2025 by health district of residence.
| Health district of residence (formerly DHB region) | Numbers | Rate per 100,000 |
| Northland | 6 | 2.9 |
| Waitematā | 26 | 3.9 |
| Auckland | 23 | 4.6 |
| Counties Manukau | 74 | 11.4 |
| Waikato | 15 | 3.1 |
| Lakes | Less than 5 | – * |
| Bay of Plenty | Less than 5 | – * |
| Hauora Tairāwhiti | 6 | 11.1 |
| Taranaki | Less than 5 | – * |
| Hawke's Bay | 5 | 2.7 |
| MidCentral | Less than 5 | – * |
| Whanganui | Less than 5 | – * |
| Capital and Coast | 11 | 3.3 |
| Hutt Valley | 5 | 3 |
| Wairarapa | 0 | 0 |
| Nelson Marlborough | Less than 5 | – * |
| West Coast | 0 | 0 |
| Canterbury | Less than 5 | – * |
| South Canterbury | Less than 5 | – * |
| Southern | Less than 5 | – * |
* Rates are not presented for districts where there were fewer than 5 cases. This is to make sure privacy and confidentiality is maintained.
The following table details the number and rates of people being admitted to hospital with rheumatic fever for the first time in 2024/2025 by health region of residence.
| Health region of residence | Numbers | Rate per 100,000 |
| Northern | 129 | 6.4 |
| Te Manawa Taki | 30 | 2.8 |
| Central — Te Ikaroa | 26 | 2.6 |
| Te Waipounamu | 9 | 0.7 |
Rheumatic fever report
Rates and numbers are available by:
- totals
- ethnic group
- age group
- health district and region.
Rheumatic fever 2024 insights report
An insights report completed in 2024, provided analysis of rheumatic fever and rheumatic heart disease through the COVID-19 pandemic in New Zealand. This work was led by Tōmaiora, researchers from the University of Auckland. Key findings included:
- significant decreases in crude acute rheumatic fever hospitalisation rates in 2021/2022
- marked inequities still persisted for Māori and Pacific peoples
- the COVID-19 elimination-suppression strategy had a significant independent effect in a best fit model, associated with a reduction in acute rheumatic fever hospitalisations by 50%.
Rheumatic Fever Roadmap 2023 to 2028
The Rheumatic Fever Roadmap has been developed to reset, renew and amplify efforts in Aotearoa New Zealand to prevent, identify and manage rheumatic fever and rheumatic heart disease. It sets out existing and new priority actions and opportunities for investment in the coming years.
The roadmap has 3 focus areas.
- Whānau Ora — determinants of wellbeing and primary prevention.
- Tāngata Ora — quality health care and improved journey through the health system for those with rheumatic heart disease and rheumatic fever.
- Kōkiri Ngātahi — system readiness and change.
These focus areas will help us:
- eliminate inequities
- meet our commitments to Te Tiriti o Waitangi
- ensure timely access to quality care
- place the needs of people with lived experience of rheumatic fever and rheumatic heart disease at the heart of our efforts.